(CNN) — Being rushed to a hospital nearly two hours away, in the middle of a dangerous spring storm – with fear in her heart and amniotic fluid leaking down her leg – was not how Ashley O’Neil expected her first pregnancy to go.
At 21 weeks pregnant, O’Neil was having some unusual vaginal bleeding. With growing worry, she and her husband, Jorge, visited the nearby community hospital in rural Maryland where she had been receiving care during her pregnancy.
Once they arrived at the local hospital, O’Neil asked to be evaluated by an ob/gyn.
“They took me right up to triage,” she said. “I was there for hours before a doctor actually came in to see me. And the whole time, my husband is yelling, ‘Where’s an ultrasound? She needs an ultrasound! What’s going on?’ ”
A physician finally entered the room where O’Neil was waiting and started to perform a vaginal exam. That’s when she saw the doctor’s jaw drop.
O’Neil’s amniotic sac, the fluid-filled structure that surrounds a growing fetus, was exposed. When someone goes into labor, the sac typically ruptures, also known as their water breaking. But with O’Neil’s sac exposed, she was at increased risk of complications, including premature rupture, possibly leading to preterm labor.
The small community hospital didn’t have the resources to support the preterm birth.
And so the frantic two-hour drive began. O’Neil was taken to a larger hospital via ground transport, as the weather was too stormy for her to be flown out, she said.
O’Neil’s experience is just one example of the challenges many mothers and babies face when living in US counties that are considered to be “maternity care deserts,” in which there is limited or no access to robust maternity care.
When O’Neil arrived at the larger hospital, her son Vinson was born preterm, at 21 weeks.
“He was born with a beating heart, 15 ounces. I like to say that he died in my arms, but I don’t think he quite made it there,” O’Neil said.
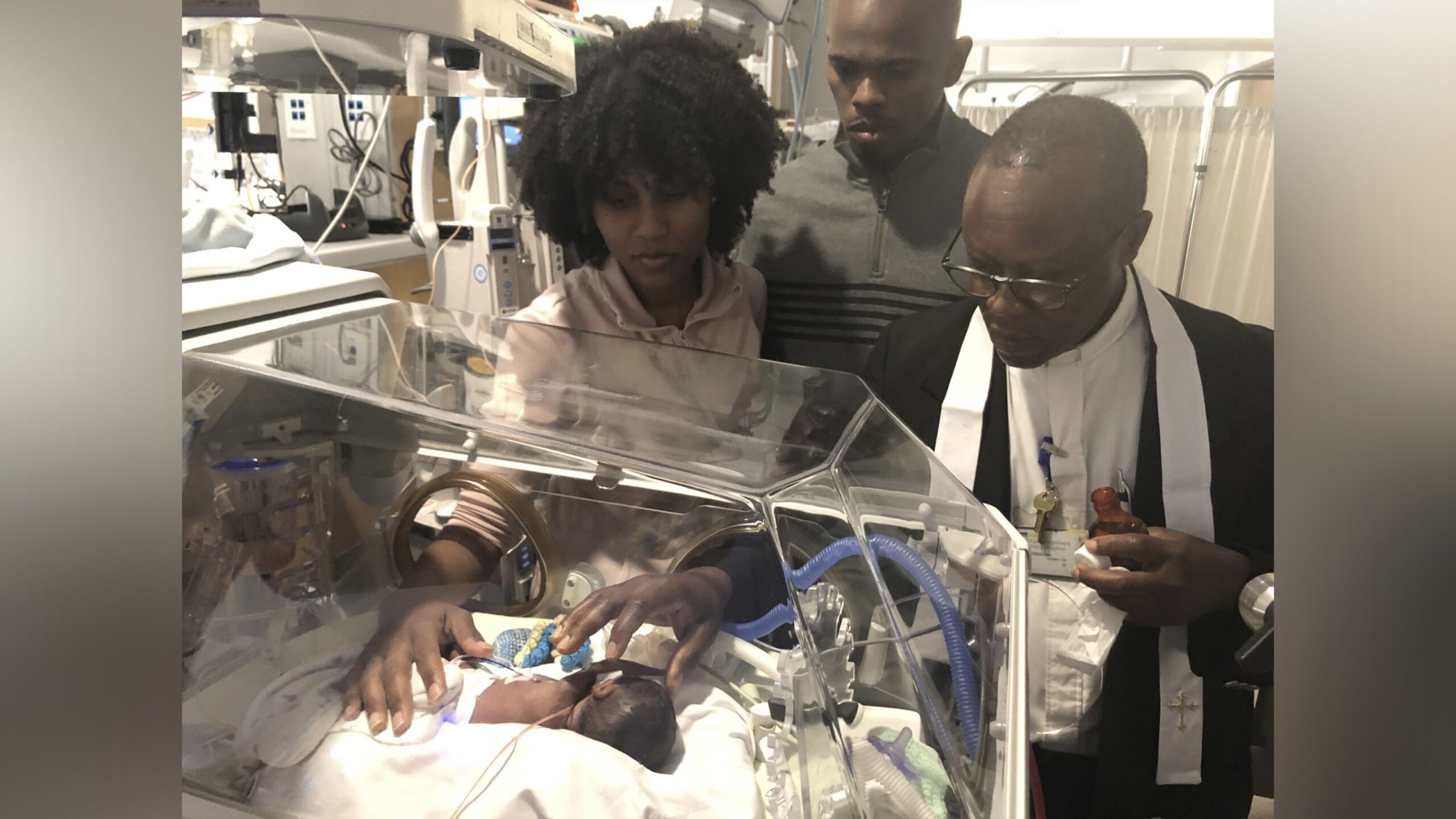
She and her husband had Vinson baptized at the hospital after he died.
Then, less than six hours after giving birth, O’Neil was wheeled through the labor and delivery unit to go home.
On the way to the exit, she could hear the cries of all the other babies in the unit.
A leading cause of babies dying
Preterm birth is a leading cause of infant deaths in the United States.
For every 1,000 babies born in 2023, about six died, according to provisional data released Thursday by the US Centers for Disease Control and Prevention. The data showed that the infant death rate last year – 5.6 deaths per 1,000 live births – was unchanged from the rate in 2022.
The rate of preterm births – in which babies are born before 37 weeks gestation – also remained at a high rate of 10.4% last year, unchanged from 2022, according to the infant and maternal health nonprofit March of Dimes.
“That means that over 370,000 babies – that’s 1 in 10 babies – are born too early,” said Dr. Amanda Williams, interim chief medical officer for March of Dimes. Racial disparities persist, she added; for Black people, the preterm birth rate is 1.5 times higher than the rate among all other babies.
In its annual “report card” on US maternal and infant health, released Thursday, March of Dimes gave the United States a D+ grade for its high preterm birth rate, marking the third year in a row in which the nation has earned that grade.
Among the 100 US cities with the highest numbers of live births, one-third were given an F grade in the report for their high rates of preterm birth last year.
Detroit had the highest rate, with 15.6% of births coming too early, followed by Cleveland at 14.8% and Mobile, Alabama, at 14.6%, according to the report.
Many of the regions with high preterm birth rates are maternity care deserts, Williams said.
“If people are unable to access care, they are not going to have adequate prenatal care,” she said. “Things like inadequate prenatal care is a major driver of preterm birth.”
To improve access to care, she added, March of Dimes supports the expansion of Medicaid, a major part of the Affordable Care Act that has been associated with lower rates of maternal deaths.
“We know that prenatal care is often coming through Medicaid, and if there is not good Medicaid policy in certain areas, then that is going to be a driver” of preterm birth rates, she said.
The US cities with high preterm birth rates also are “areas where there are many chronic conditions and patients living with a greater number of things like hypertension, diabetes, obesity – those are all drivers of preterm birth as well,” Williams said.
The cities in the report with the lowest preterm birth rates were Ramapo, New York, at 5.2% and Irvine, California, at 7% – both were given A grades – followed by Gilbert, Arizona, at 7.8%, which earned an A- grade.
‘We’re not making any headway on this’
The high rates of preterm birth that persist in the United States are a “travesty,” said Lori Tremmel Freeman, chief executive officer for the National Association of County and City Health Officials, who was not involved in the March of Dimes report.
“It’s a travesty that as a developed nation, we have these extraordinarily poor outcomes around maternal morbidity and mortality, infant prematurity and deaths, and that the disparities continue and are wide with regard to White people and Black and Brown people. We’re not making any headway on this, and we need some really targeted prevention tactics and other services to address this,” Freeman said.
“It is a complicated issue, because this involves both ensuring that a new mom is cared for, not only during her pregnancy, but that she comes into the pregnancy healthy,” she said. “Often in rural and other economically disadvantaged areas, they don’t have the providers in place. It’s hard to get access to health care. It’s hard for working mothers to get to prenatal care. So there’s a lot of contributing factors here, and it’s going to take the whole of the health system – including public health and health care – to actually turn the corner and reverse some of these outcomes.”
To improve the state of maternal and infant health and to lower rates of preterm birth, March of Dimes has recommended that more states provide 12 weeks of paid family leave, require Medicaid to reimburse for doula care, develop committees to review and study maternal and infant deaths and expand access to midwives, among other actions.
“We know that when a low-risk pregnancy is supported by a midwife, that it is associated with lower risks of preterm birth,” Williams said.
Some research suggests that midwifery care could reduce about two-thirds of maternal and infant deaths and significantly decrease risks of severe complications associated with pregnancy or childbirth, said Amanda Shafton, the national midwifery director of Ob Hospitalist Group.
“In the United States, there are only 4 midwives for every 1,000 live births, while other high-income countries see between 30-70 midwives per 1000 births. The countries with the lowest maternal mortality rates are those who prioritize midwifery-based care, with the vast majority of babies being delivered by midwives,” Shafton, who was not involved in the March of Dimes report, wrote in an email.
“To actively involve nurse-midwives in the fabric of obstetrical care in the United States, changes are needed across the board,” she said. “It’s essential to advocate for hospital bylaw changes, increased opportunities for collaboration between midwives and OB-GYNs, and updated regulations on state and federal levels to allow nurse-midwives to practice to the fullest extent of their education and licensure.”
Shafton added that it’s important to “increase the midwifery workforce” and “achieve equitable payment models” for midwives, from public and private insurance as well as individual salaries.
March of Dimes also recommends that pregnant people discuss the benefits of low-dose aspirin with their providers to reduce the risk of preterm birth, especially if they’re at higher risk of a dangerous condition called preeclampsia.
“It is absolutely probably my favorite and most impactful intervention, because it’s so simple. You can go to your local pharmacy and purchase over-the-counter 81-milligram low dose aspirin and take it with prenatal vitamins every day from about 12 weeks to the end of pregnancy to decrease preeclampsia and preterm birth in patients who are at risk for preeclampsia,” Williams said.
“What we encourage is that all patients get educated about it. All prenatal care providers screen for it. And if the patient is at risk, and many patients are, then they take it on a daily basis, from approximately weeks 12 through the end of pregnancy,” she said. “There are many different risk factors that should be discussed with one’s prenatal care provider.”
Those risk factors include being older than 35, using in vitro fertilization, being of Black race due to exposure to the stress of systemic racism, having a low income, experiencing your first pregnancy, having twins or triplets or already having a chronic health condition like high blood pressure.
Telehealth also could be a way to help expectant mothers, O’Neil said.
“Every pregnant woman who lives in a maternal health care desert should be provided with access to a health care app that is monitored by remote providers. In this app, she can track how she is feeling and if she is having any symptoms like edema or headaches. She can ask questions,” she said.
“I also think that they should go home with a blood pressure machine,” she said, especially those with an increased risk of preeclampsia. “So they can input their vitals daily, and the system can alert providers when the readings are outside the normal parameters. In addition, utilizing mobile health vans to conduct prenatal visits is crucial in increasing access.”
‘I’ll fight for as long as you want’
O’Neil said she sees it as her calling to raise awareness around preterm birth and the solutions needed to reduce the risks.
Shortly after giving birth to Vinson preterm in May 2016, O’Neil became pregnant with her second son, Kolin. In April 2019, Kolin was born at the same small community hospital where O’Neil was seen during her previous pregnancy.
With her second pregnancy, the hospital again wanted to transfer her to the larger hospital – but it was too late. “The labor came too quick,” O’Neil said.
She had an emergency C-section.
“When I woke up from surgery, I was scared to look around or ask, ‘Where’s my baby?’” O’Neil said.
Kolin was delivered preterm, but the medical team was unable to intubate him. “They gave him manual breaths for an hour, until the flight came to transfer him,” O’Neil said.
Kolin was transferred to NICU at the larger hospital, two hours away.
“We didn’t know that he was going to make it,” O’Neil said.
While visiting Kolin in the NICU, she whispered to him, “ ‘Look, if you want to go, you can go, but if you want to fight, I’ll fight for as long as you want to fight.’ ”
Kolin survived and came home six months later.
He was diagnosed with cerebral palsy, along with other conditions, and he has a feeding tube. But O’Neil said his diagnoses don’t keep him from enjoying life. With specialized care, physical therapy and speech therapy, her son has been thriving.
But shortly after O’Neil’s family celebrated Kolin coming home, they faced another tragedy: the death of O’Neil’s husband, Jorge.
“In a four-year span, my son died, my second son was born four months early, spent six months in the NICU, and then my husband died four years from the same month as my first son died,” O’Neil said.
In her grief, O’Neil focused on uplifting other NICU families by launching a podcast called “Ask a NICU Mama” and writing a book titled “It’s a NICU World.”
O’Neil’s mission has been to show that if she can “survive and not go completely crazy,” others can find hope too, she said. “I know life can get dark and heavy and feel like you’re suffocating at times, but I just want to show that if I can make it, so can someone else.”
After she had two premature births three years apart – with one resulting in her elder son’s death and the other leaving her younger son with lifelong disabilities – the nation’s ongoing high preterm birth rate breaks her heart, O’Neil said.
“When a child is born prematurely, it does not just affect that child or that family, but it affects our society as a whole. Do you know how many resources are used in order for my child to thrive? Raising him takes so much of me, in ways that mothers of neurotypical children could never understand,” O’Neil said.
“I had to leave my job as a family nurse practitioner working in a busy, understaffed medical clinic because my son needed me at home. All of his medications, therapies, surgeries, et cetera, come at a high financial cost,” she said. “We supposedly live in the greatest country in the world, and yet every day as a country, we fail pregnant women and their babies.”
The-CNN-Wire



